- Jeanne Gray
Medical Marijuana For Anxiety - Benzos VS Weed
The following describes my personal experience with benzodiazepines, a class of tranquilizers that effectively relieves anxiety and muscle tension. In fact, “benzos” work so well that the body quickly accommodates them, often leaving a person physically addicted when drug abuse is not intended. During acute withdrawal, beside the “rebound” anxiety and insomnia, one is at risk for seizures, heart attacks, and suicidal ideation. Stopping “cold turkey” can kill the user who is trying to get “clean”. The harrowing phases of withdrawal can last weeks, months and in some cases, years.1
My story is not intended to diagnose or treat others, as I am not a medical professional. I have, however, learned enough from decades on psychotropic prescriptions to issue a cautionary word about the most common pharmacological treatment for anxiety. Gladly, I found medical marijuana safely alleviated my symptoms so I could focus on living.
Anti-Anxiety (“Anxiolytic”) Drugs & Chemical Dependency
As excruciating as physical withdrawal can be, psychological dependence often takes significantly longer to unwind for three key reasons:
1. The emotional buffering benzos provide eases emotional discomfort, something most humans naturally crave at one time or another.
2. The common side effect of memory loss not only impedes the growth and nurturance of existing interpersonal relationships, but also inhibits the formation of new memories. The user who does not remember the adult-appropriate commitments he has made because he is “missing” that segment of time will be hard-pressed to follow through on those obligations. Such gaps in awareness further erode credibility with others and with the addicted person.
3. The dysfunction that prompted the person to seek relief in the first place if not dealt with, comes out of “deferment.” For example, a person with post-traumatic stress disorder (PTSD) will likely continue to fight flashbacks or night terrors unless he has faced the underlying traumas, de-fusing them through alternate therapies such as behavioral modification, Eye Movement Desensitization and Reprocessing (EMDR) or more recently, Lifespan Integration (LI)™ Therapy.2
Cannabidiol (“CBD”), one of dozens of cannabinoids found in the Cannabis sativa plant, is nonpsychoactive (does not get you high) and not addictive. On this site you will find links to purchase hemp-derived CBD to try for yourself. As with any substance you ingest, always use due diligence, verifying that the oil is independent third-party lab-tested, sourced from organic farms, free of pesticides, and (ideally) grown in a “legal” state like Washington, Colorado, or California. Hemp from China or eastern Europe, grown for manufacturing textiles, plastics or biofuels, contains only trace CBD. Cannabidiol extracted from industrial hemp rather than marijuana is legal in all 50 states because it does not fall within the jurisdiction of the DEA, unlike its cousin, THC-rich cannabis.
In the state of Florida an adult can legally order CBD online. You will need a doctor’s authorization, however, to use medical marijuana with THC, or even CBD isolate if it has been derived from the marijuana plant. Due to a paucity of research in America—given cannabis’ unfortunate classification as a Schedule I narcotic—the therapeutic dose of CBD for treating anxiety has not yet been determined, but research into this use of CBD and subsequent data for dosing looks promising.3 Side effects of dry mouth or lightheadedness are usually minimal, and tolerated well.
My Story About How Marijuana Replaced Traditional Medications
The road to chemical dependency started innocently enough. I grew up in an emotionally unpredictable home. While a sophomore in college, a panic attack crept up on me. While trying to talk with an academic advisor about my “checking out” (dissociating) during class, I found myself scraping my thumb till it bled, just to feel something. Before I realized what was happening, Campus Security had transported me to a local psychiatric hospital for overnight evaluation on a precautionary stay, due to the self-harm. Late that night the nurse offered me, a seasoned insomniac, something to “calm my nerves” and I said, “Yes.” Just like that, Xanax became my new best friend.
The next three years I continued to use Xanax (alprazolam) intermittently for anxiety. The prescription helped at first, but my use quickly got out of hand. The next three decades my family and a few close friends saw a young lady struggling to find herself. I earned dual degrees in college, but everyday living baffled me. In a recurring cloud of depression, I visited over a dozen counselors for help “staying on track.” My doctors prescribed Ativan (lorazepam) for panic, Klonopin (clonazepam) for stress, and Valium (diazepam) for muscle tension. I would use them as prescribed for a few weeks, then take them whenever I wanted, then back off, keeping the cycle of addiction turning.4 Perpetually on a diet to lose weight, I preferred prescriptions over alcohol, because they had fewer calories.
Ironically, as of this writing, the Food and Drug Administration (FDA) still officially considers cannabis a Schedule I drug, with purportedly “no potential medical benefit,” while benzodiazepines are Schedule IV drugs, with a “low potential for abuse.” I take issue with such an archaic classification system, because common sense, decades of case studies, and an increasing number of scholarly research studies demonstrate that the reverse is true: cannabis (whether CBD alone or in conjunction with THC) is significantly safer for the patient than benzodiazepines.
I justified my self-medicating as necessary while trying to face down the demons I’d tolerated since childhood. Who could know how long recovery would take? When the path to wholeness seemed impossibly steep, I retreated. The tranquilizers I absorbed daily had quelled not only my anxiety but also my desire to push my own boundaries, engage new endeavors and grow as a person.
Functional Addict
While I carried on mothering our children and holding other adult responsibilities, the prescription drug abuse continued through 1999, on the verge of “Y2K” when I thought the world as we knew it would slide into a morass of dystopia. (The use of mood-altering medications had left me more than a little paranoid.) My world almost did devolve, as my addictive behaviors escalated. An elderly psychiatrist had prescribed me four 10-mg Valium a day and Xanax “as needed,” which to me meant quite often.5 When he hesitated to prescribe two benzodiazepines I assured him I was aware of the risks and would only use them when necessary. Besides, I told him, “Low doses don’t affect me," which was actually true, as my system had grown nearly impervious to standard dosages. Unbeknownst to him, I already possessed a few dozen bromazepam (mid-length duration benzo) I had imported from Thailand. I hoarded each new prescription as though collecting precious jewels.
In 2001 my elderly psychiatrist retired, and my new one, Dr. H., prescribed cautiously. In silent protest I decided to take matters further into my own hands. When he briefly left the room, I pocketed a blank slip from the prescription pad he had left on the counter. For the next few weeks I went on a forging spree, in hindsight, to get caught. I had grown weary of the dangerous game I was playing, and became more than a bit cocky.
One day I upped the ante by trying a new pharmacy for an additional stock of pills. The staff saw me lingering nearby waiting for the order to be filled, so they called my psychiatrist to verify that he had written the orders. The pharmacist confronted me, saying my doctor had opted not to have me arrested right there. Instead I was to report to his office the next day to “work things out.” Once we were face-to-face, he gave me an ultimatum: get “clean” and enter a 30-day residential treatment center or go to jail. I chose the detox-and-treatment route. The next seven days at a local hospital involved clearing my system of the tranquilizers, a painful and dangerous process due to the high risk of seizures.
I got to go home for one day before entering the residential facility. When I took a shower the water felt like a thousand barbs, lights seared my eyes, sounds echoed and my limbs repeatedly seized up with involuntary contractions. In short, all the systems the anti-anxiety medications had suppressed for years went into overdrive.6 As terribly as I missed our daughters (aged 9 and 5) my husband had flown to Alaska during the week-long inpatient detox, I was glad they did not see me in such a pained condition.
“Clean” from benzodiazepines for nine years, I tried again to use them responsibly in 2010, when I also started counseling with a reliable psychotherapist. I had grown more aware of my impact on our children, aged 18, 14, eight and three years old. They needed my mind as well as my body to be available as they negotiated the challenges of childhood. Meanwhile my new psychiatrist and I chose to keep the anxiolytics’ dosages minimal, and I agreed not to take them daily. Still I wondered whether taking any prescription drugs was worth the risk of getting addicted all over again. I loathed the notion of causing collateral damage to those I love.
Enter Medical Cannabis, a less “Sticky” Alternative

In July of 2014, Washington state recreational dispensaries opened for business. That September, aware of the recent media attention on cannabis, I began reading up on medical cannabis or “MMJ”, which had been legal in Washington since 1998. The conditions qualifying for a medical recommendation included the PTSD I faced, as a debilitating condition that had “significantly interfere(d) with the patient's activities of daily living and ability to function.”7 I had tried smoking street pot once in the late 1980s and felt paranoid for two days, steering clear of that drug ever since. I already felt enough anxiety.
Yet now I read online dozens of anecdotal reports of CBD-rich strains of cannabis alleviating the symptoms of a host of illnesses. I had heard some strains affected cancerous tumors, the devastating seizures of epilepsy, and had shown promise in relieving muscle spasticity in patients with multiple sclerosis. In autumn 2014, I learned that hundreds of different strains were now available—how growers of all levels of experience were producing new cross-breeds. I read that several hybrids had helped many others quell the symptoms of chronic anxiety or PTSD. Since I was concurrently seeking effective counseling for the issues underlying my long-term anxiety and insomnia, I decided to give modern, medical cannabis a try. Perhaps, I thought, MMJ could completely supplant benzodiazepines so I’d never have to put my life or anyone else’s at risk again.
The first time I walked into a medical dispensary I felt vaguely guilty, as though I were doing something sneaky again, then reminded myself I had a medical authorization in hand—one I had not written for myself. The receptionist checked my authorization, then remotely unlocked the door for me to enter. I passed through a neon-lighted hallway, then through a curtain of hanging beads. I entered a hippie-friendly low-ceilinged room which smelled distinctly of skunk. I plugged my nose and winced, asking the bud-tender, “What is that smell? Is that weed? Eek!”
The good-natured bud-tender grinned in the affirmative and chuckled at my obvious newbie status. (I find the scent of dried cannabis is an “acquired smell.”) The staff delightedly took turns informing me of “what’s what” in the wide world of Seattle’s pot culture. Along with cannabis “flower” for smoking, the staff showed me vape cartridges, CBD capsules, candies, topical treatments, even infused coffee. An hour later I left the dispensary with a few grams of cannabis, three awful-tasting but potent fudgey “chews” and more than an ounce of friendly advice.8
Suddenly I found a sense of community I had previously only experienced at our church, during worship. What a drastic switch! Using anti-anxiety pharmaceuticals, I had withdrawn from others, further isolating with each increase in dosage. The anxiolytics turned off not only my difficult feelings, but also dulled my capacity to experience joy, humor, sense of adventure, and most importantly, my spiritual connection with God. After visiting a few dispensaries and using all the “new patient” deals I could find, I excitedly headed home to try the various products. In the car, before even trying a sip of infused lemonade, I already felt happier than I had in years.
Trying Everything
Over the next several months I felt like a kid in a candy store. I experimented with extracts, baked ultra-high dose, low-sugar medicated edibles (dubbed “medibles” by the local cannabis community), even juicing the raw leaves (which tasted like lawn clippings, but cleared my acne and sweet tooth, but that is a story for another day). My children did not like the smell of decarboxylating cannabis, but they put up with it. In return, they encountered a more sociable, more real mom—one the anxiety (then anti-anxiety meds) had for years distorted or masked entirely. My humor returned, as I no longer took myself and my plight so seriously. Frequenting the MMJ dispensaries, I had held the door open for patients in wheelchairs, dealing with other chronic medical handicaps. I no longer took my physical health for granted. Sure, my self-defeating thinking patterns needing adjusting, but I finally considered therapy a quite doable endeavor.
Since I don’t like smoking, I stuck with edibles. I tried coconut oil-capsules with CBD-rich strains like ACDC, Harlequin or Cannatonic.9 Once I got over my amusement at the names of the strains, I recognized that the fact that this plant comes in so many varieties means it likely holds tremendous potential for a variety of ailments. The rumors of this plant disrupting “Big Pharma” were true! I could foresee the cannabinoids, in various admixtures, someday not only replacing many prescription medications, but also preventing disease. Cannabis grabbed my attention.
After about 45 minutes I felt the anxiety and muscle tension melt away, and emotionally drawn toward other people instead of away from them. In addition, I found myself “present” when my husband wanted to have sex, a welcome change from my previously disaffected stance toward his advances. (Early SSRI anti-depressants had eradicated my libido for years.) Now even my skeptical husband was on board with this new plant-based medicine—one that gave him back his wife!
An avid gardener, I soon started my own “grow” with clones (young cannabis starts) of 15 plants, including “fun” strains like Juicy Fruit, Grape Romulan and Maui Wowie (or Waui). The garden, in individual grow bags, smelled fantastic. With dinner in the oven, or clothes in the dryer, I would head to our backyard for a break. I sat on our porch swing petting Twig our rescued bunny, simply enjoying the crisp fall air. Whether “on” medical marijuana at the moment or not, I found I could relax for the first time in years. I could take a coco-cap(sule) of a hybrid strain (or a typically “daytime” Sativa) and proceed with my day. I was a much safer driver during those early months of trying MMJ than I had been on any of the sedatives I had been prescribed for years. Still, I don’t recommend driving under the influence of any perception-altering substance.
Finally, A Manageable Solution
Through a meandering series of events I ended up using medical marijuana instead of benzodiazepines for PTSD, and now only for occasional anxiety or insomnia. By the grace of God, and with professional help, I am alive and enjoying life. I now have an arsenal of coping tools to deal with everyday stress, with the past firmly rooted behind me. I’ve heard it said, “The past and the future are great places to visit, but I don’t want to live there.”
In an ideal world our neurotransmitters would work in perfect synchrony, but we humans have so thoroughly tampered with creation that many of us now need a chemical assist to function in society. Unfortunately, in my case, as with many other Americans, the pharmaceuticals typically prescribed for anxiety led to iatrogenic depression and chemical dependency. If you are stuck in the trap of addiction, let me assure you that hope exists outside your own mind.
Cannabidiol is not a panacea for all ills. Life is not nearly so black and white, thank God. Nonetheless, both CBD, a powerful nonpsychotropic chemical, and medical marijuana deserve consideration. Both have proven themselves robust treatments for many of the maladies we’ve come to assume can only be fought with prescription pharmaceuticals. I propose that If you suffer from chronic anxiety as I did, CBD or CBD-rich cannabis may provide you more organic and lasting relief from your symptoms, to get you back to living.
______________________________
1 Pfaff, Robert. “The Gauntlet of Protracted Benzodiazepine Withdrawal.” Mad In
America, 23 July 2017, www.madinamerica.com/2016/01/the-gauntlet-of-protracted-benzodiazepine-withdrawal/ (accessed March 2, 2018).
2 Pace, Peggy. “The Neuroscience of Lifespan Integration™ Therapy.”
Lifespan Integration™ lifespanintegration.com/neuroscience-lifespan-integration-therapy/, excerpted from Pace, P. (2015) Lifespan Integration: Connecting Ego States through Time. Eirene Imprint.
3 “Can Cannabis Replace Benzodiazepines as an Anti-Anxiety Drug?” Royal Queen
Seeds, 7 July 2017, www.royalqueenseeds.com (accessed March 3, 2018)
4 “Benzodiazepine Addiction Rates.” www.blackbearrehab.com
(accessed March 6, 2018)
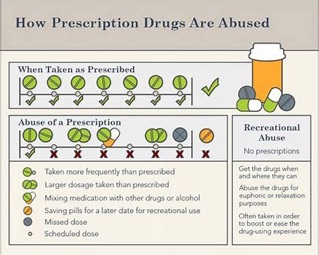
5 “How Prescription Drugs Are Abused.” Benzodiazepine Addiction Treatment,
www.americanaddictioncenters.org (image accessed March 6, 2018)
6 “Benzodiazepine Withdrawal Symptoms, Timeline and Effects.” Withdrawal.net, American
Addiction Centers, www.withdrawal.net/learn/benzodiazepine-symptoms-timeline-effects/ (accessed March 7, 2018)
7 “You and Your Family.” Washington State Department of Health,
www.doh.wa.gov/YouandYourFamily/Marijuana/MedicalMarijuana/PatientInformation/QualifyingConditions (accessed March 2, 2018)
8 Author’s Note: Cannabis dispensaries of 2018 barely resemble their “Wild West”
predecessors of 2014. Carefully regulated by state laws, modern “pot shops” in Washington state and Colorado appear professional and well-lighted, with ATMs at hand, so you don’t have to arrive with a “fistful of dollars.” Gone are the days of bud-tenders serving up an order out of a pickle jar on the counter. The cannabis is pre-weighed and packaged, all inventory from “seed to sale” meticulously tracked. Instead of hand-written descriptions, the “menu” at a dispensary typically includes the cannabinoid and terpene (aromatic component) profile of each strain. A patient (or customer, in legalized states) no longer needs to guess what’s in the bud she buys.
9 “CBD For Anxiety: 5 Fascinating Benefits” Hempworx, 1 Oct. 2017,
greencamp.com/cbd-for-anxiety (accessed March 6, 2018)
#medicalmarijuanaforanxiety #benzodiazepinesvsmarijuana #antianxietydrugs #cbdandmedicalmarijuana #cannabidiol #cannabinoids #marijuanalaws #floridamedicalmarijuana #xanax #medicalmarijuanaforPTSD #medicalmarijuanaforpain

